Frequently Asked Questions
Find answers to our application process
New Hire Appointments
I need to reschedule my new hire appointment.
1. Log into your candidate account.
2. Click 'Go to my jobs' in the upper left, choose 'Prepare for your Appointment' and find the job you are applying for.
3. This will display your pre-hire checklist for this job.
4. At the top of the screen, you will see a banner with the date and time for your pre-hire appointment.
5. To reschedule your appointment, click the ‘Reschedule’ link next to ‘Can’t attend at this time?’.
2. Click 'Go to my jobs' in the upper left, choose 'Prepare for your Appointment' and find the job you are applying for.
3. This will display your pre-hire checklist for this job.
4. At the top of the screen, you will see a banner with the date and time for your pre-hire appointment.
5. To reschedule your appointment, click the ‘Reschedule’ link next to ‘Can’t attend at this time?’.

6. Now you will be able to review the available appointments that will allow you to keep the same shift and start date (Day 1) schedule.
If you need more help, please choose an option above to connect with candidate support by phone, chat or text.
If you need more help, please choose an option above to connect with candidate support by phone, chat or text.
I am trying to schedule an appointment, but there are no appointments available.
New hire appointments fill up quickly! We load jobs as soon as they come available. Please continue to check your job page daily for future appointment openings.
1. Log in to your candidate account
2. Click on the menu in the upper right hand corner
3. Click on 'Jobs I've Applied To.' You will then be able to click on 'Please continue your application' to pick from available hiring appointments
Note: If there is nothing available, it means that all of the slots have filled up. We encourage you to check your application frequently in the event of more openings.
1. Log in to your candidate account
2. Click on the menu in the upper right hand corner
3. Click on 'Jobs I've Applied To.' You will then be able to click on 'Please continue your application' to pick from available hiring appointments
Note: If there is nothing available, it means that all of the slots have filled up. We encourage you to check your application frequently in the event of more openings.
I am trying to schedule an appointment but am unable to attend any of the available appointments.
All available appointments will be shown on the job page. If you are unable to make any of the available appointments, please continue to check your job page daily for future appointment openings. To check for available appointments, follow these steps:
1. Log in to your candidate account
2. Click on the menu in the upper right hand corner
3. Click on 'Jobs I've Applied To'
You will then be able to click on 'Please continue your application' to pick from available appointments.
1. Log in to your candidate account
2. Click on the menu in the upper right hand corner
3. Click on 'Jobs I've Applied To'
You will then be able to click on 'Please continue your application' to pick from available appointments.
I had a new hire appointment in the past, but could not attend and need to reschedule.
A new hire appointment is your initial appointment after you have applied.
In order to reschedule your new hire appointment please follow these steps:
1. Log in to your candidate account
2. Click on the menu in the upper right hand corner
3. Click on 'Jobs I've Applied To'
4. Under 'My Appointments', click on the 'Action' button next to your scheduled appointment
5. Click on 'Cancel'
6. Refresh your page and click 'Please continue your application'
7. You can now select your shift preferences and schedule a New Hire Appointment. If there are no appointments available, you will not be able to reschedule your appointment at this time.
In order to reschedule your new hire appointment please follow these steps:
1. Log in to your candidate account
2. Click on the menu in the upper right hand corner
3. Click on 'Jobs I've Applied To'
4. Under 'My Appointments', click on the 'Action' button next to your scheduled appointment
5. Click on 'Cancel'
6. Refresh your page and click 'Please continue your application'
7. You can now select your shift preferences and schedule a New Hire Appointment. If there are no appointments available, you will not be able to reschedule your appointment at this time.
Login Issues
How do I reset my account PIN?
To reset your personal PIN, go to https://hiring.amazon.com/app#/forgotPin. Type the email address you used when you made your account and click 'Next'.

You will get an email with a verification code. Copy and paste the code into the first empty space. Choose a new 6-digit pin that you can remember and type it into the next two blank spaces. Click 'Update'.

I forgot the email address or phone number I used to create my account.
To log into your account or reset your password PIN, you need to know the email address and the phone number you used when you set up your account.
If you cannot remember what email address you used or if you did not verify your mobile phone number when you made your account, connect with candidate support by phone, chat or text.
If you cannot remember what email address you used or if you did not verify your mobile phone number when you made your account, connect with candidate support by phone, chat or text.

How do I create an account?
You can sign into your profile to confirm or change your information at any time.
To view your personal information:
1. Log into your account at https://hiring.amazon.com/app#/login.
2. Click 'Edit' next to 'My Personal Information'.
3. This takes you to the Edit Profile page, where you can review your information.
To edit your information:
1. Choose the part you want to update.
2. After you expand the section, the edit option will be available in the right corner.
3. If you make any changes, click 'Save'.
If you do not see the information you want to change, connect with candidate support by phone, chat or text for more help.
To view your personal information:
1. Log into your account at https://hiring.amazon.com/app#/login.
2. Click 'Edit' next to 'My Personal Information'.
3. This takes you to the Edit Profile page, where you can review your information.
To edit your information:
1. Choose the part you want to update.
2. After you expand the section, the edit option will be available in the right corner.
3. If you make any changes, click 'Save'.
If you do not see the information you want to change, connect with candidate support by phone, chat or text for more help.
I received a message saying “My email is already registered…”
If you got the following message: “This email is already registered. Please provide a different number or login with this email address,” this means you already have an account in our system!
To continue, log into your exiting account. To reset your password pin, go to https://hiring.amazon.com/app#/forgotPin.
If you did not create an account before, make sure you typed your email address correctly. If this does not solve the problem, connect with candidate support by phone, chat or text for more help.
To continue, log into your exiting account. To reset your password pin, go to https://hiring.amazon.com/app#/forgotPin.
If you did not create an account before, make sure you typed your email address correctly. If this does not solve the problem, connect with candidate support by phone, chat or text for more help.
I need to confirm or edit information on my profile.
You can sign into your profile to confirm or change your information at any time.
To view your personal information:
1. Log into your account at https://hiring.amazon.com/app#/login.
2. Click 'Edit' next to 'My Personal Information'.
3. This takes you to the Edit Profile page, where you can review your information.
To edit your information:
1. Choose the part you want to update.
2. After you expand the section, the edit option will be available in the right corner.
3. If you make any changes, click 'Save'.
If you do not see the information you want to change, connect with candidate support by phone, chat or text for more help.
To view your personal information:
1. Log into your account at https://hiring.amazon.com/app#/login.
2. Click 'Edit' next to 'My Personal Information'.
3. This takes you to the Edit Profile page, where you can review your information.
To edit your information:
1. Choose the part you want to update.
2. After you expand the section, the edit option will be available in the right corner.
3. If you make any changes, click 'Save'.
If you do not see the information you want to change, connect with candidate support by phone, chat or text for more help.
Application and Hiring Process
How do I apply? Can I re-apply?
You can see all of Amazon’s open Warehouse, Shopper, Air, and Driver positions on our site.
Availability is constantly changing, and we encourage you to check our site frequently for updates. You can also sign up to receive job alerts either by texting NEWJOB to 31432 or sign up for email alerts.
Note: If you don’t see a job posting for a particular location, it means that all of the roles have been filled.
Availability is constantly changing, and we encourage you to check our site frequently for updates. You can also sign up to receive job alerts either by texting NEWJOB to 31432 or sign up for email alerts.
Note: If you don’t see a job posting for a particular location, it means that all of the roles have been filled.
Why don't I see any jobs in my area?
If you don’t see jobs near you, sign up for mobile alerts by texting NEWJOB to 31432. If you’re only interested in driver roles, text DRIVENOW to 31432.
You can also sign up for email alerts at amazon.com/tc.
"STOP" to opt-out. T&C/Privacy Policy here.
You can also sign up for email alerts at amazon.com/tc.
"STOP" to opt-out. T&C/Privacy Policy here.
What is my application status?
You can check the status of your application by following these steps.
1. Log in to your candidate account
2. Click on the menu icon in the upper right hand corner
3. Click on 'Jobs I've Applied To' from the dropdown menu
4. You will see your appointment details under the "My Appointments" section
1. Log in to your candidate account
2. Click on the menu icon in the upper right hand corner
3. Click on 'Jobs I've Applied To' from the dropdown menu
4. You will see your appointment details under the "My Appointments" section
What is your hiring process?
For Customer Service roles, visit this link.
For our warehouse jobs, this is how our hiring process works:
Step 1 - Application
Our online application can be completed in about an hour and includes picking your shift and scheduling your new hire appointment.
Step 2 - New Hire Appointment
This is where you complete the hiring process. You’ll need to provide proof of your identity and employment eligibility.
Step 3 - New Hire Orientation
Learn about your new job, hear from senior leaders, and get your badge photo for your first day.
Step 4 – Your First Day
At Amazon, we call your first day on the job "Day 1."
Learn more about Amazon's hiring process.
For our warehouse jobs, this is how our hiring process works:
Step 1 - Application
Our online application can be completed in about an hour and includes picking your shift and scheduling your new hire appointment.
Step 2 - New Hire Appointment
This is where you complete the hiring process. You’ll need to provide proof of your identity and employment eligibility.
Step 3 - New Hire Orientation
Learn about your new job, hear from senior leaders, and get your badge photo for your first day.
Step 4 – Your First Day
At Amazon, we call your first day on the job "Day 1."
Learn more about Amazon's hiring process.
Do I need a resume?
Most hourly jobs at Amazon do not require a resume, including warehouse, driver, and shopper jobs! If you're applying for a job at a campus pickup point job, you will need to provide a resume.
Do I need to interview?
Our hiring process for most hourly roles does not include an interview!
If you are applying for delivery driver role, you will be required to interview as part of your hiring process.
If you are applying for delivery driver role, you will be required to interview as part of your hiring process.
Why was my application rejected?
Amazon reviews a variety of things when determining which candidates to move forward in the hiring process. Some of the details we review include your work history, the questions you answered during the application process, and the results of your background check and drug test. We cannot give details about these factors.
Do I need to complete my application or can I come back to it later?
You must finish your application within 3 hours, otherwise, we cannot guarantee you keep your selected shift.
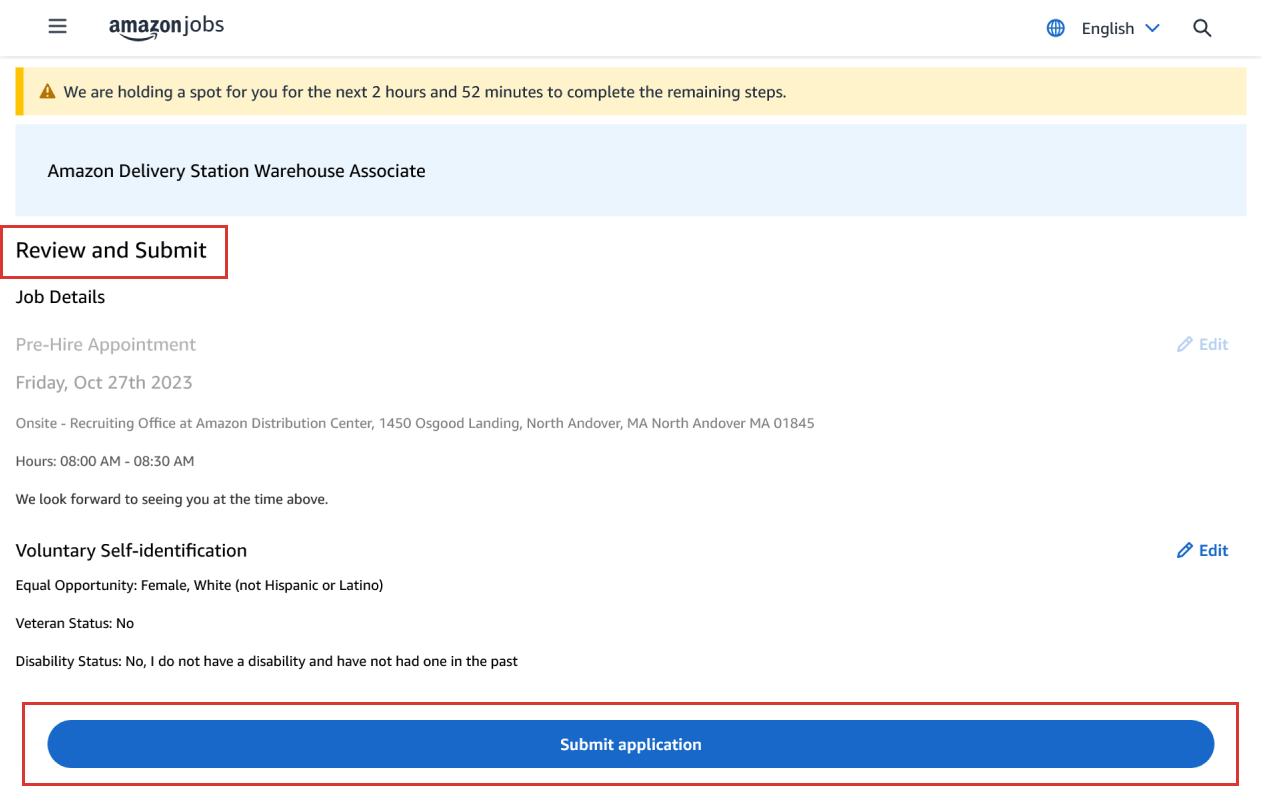
How do I know I’ve completed my application?
Once you’ve selected a new hire event, you'll be on the "Review and Submit" page. Here, you'll click "Submit application" at the bottom of the page. Until you’ve finished these steps, your application is incomplete.
Rehire Process
Can I re-apply and be rehired?
If you previously worked at Amazon, you are welcome to re-apply. We will evaluate your rehire eligibility based on your employment record. Please note, all candidates who have previously been hired at Amazon will go through this check, whether they worked or withdrew before starting. Once we have finished this process, we will notify you with next steps.
How long do I have to wait before I can re-apply?
You can re-apply at any time, at which point the time when you will be eligible for rehire will be determined.
What if I was terminated or fired?
Depending on the reason behind your termination, you may not be eligible for rehire until 90 days or more after your termination date.
Do I have to return to the same shift or site that I was previously in?
You can apply to any site and role pending your rehire eligibility and job availability. It is important to note that Amazon Air Associate jobs have additional hiring requirements.
Will my benefits remain the same?
If you left and return within the same month, no new health benefit elections are required and are automatically covered as they were prior to leaving. If returning outside of the same month, new coverage elections are required. If you return within the same calendar year and elect the exact same plans, then the deductible is re-instated. Lifetime maximum benefits, fertility, hearing aids, orthodontia, wigs, and so on, do not start over upon rehire. The benefit spending will pick up at the same spot of amount spent when exiting Amazon. If you return within 6 months of your last day, you will accrue vacation at the same rate prior to leaving Amazon. If returning longer than 6 months from your last day, you will accrue vacation at the normal rate for new employees in your first year back.
Will my vacation remain the same?
If you return within 6 months of your last day, you will accrue vacation at the same rate prior to leaving Amazon. If returning after 6 months from your last day, you will accrue acation at the normal rate for new employees in your first year back.
Why can't I re-apply?
While we do not have answers directly related to applications, you can check your eligibility by logging in to hiring.amazon.com. It will notify you of your status or how long until you can apply again.
Does my UPT start over?
You receive 10 hours of UPT. If you had UPT when you left, you will get that back.
Do any of my old write-ups get put on my record when restarting?
You start with a fresh slate. No feedback.
Do I get a new badge? I have my old one still, will that work? Can I take a new badge photo?
You receive and a new badge and can request a new picture.
I used to work as a Blue Badge but now only Seasonal is available. How do I get back to a Blue Badge role?
Blue Badge positions might not currently be available. Please search jobs here and sign up for job alerts to find your desired role.
I don't want to work in my old process path. How can I make sure I don't get that department?
While things are subject to change based on your background check results, how long they take to come back, and training capacity, you are able to choose and know your department assignment prior to showing up to your first day.
Do I get new safety shoes?
You are eligible for new safety shoes.
Alumni Resources
Can I chat with MyHR and/or see previous pay statements?
Redownload the AtoZ app to access these, along with additional resources, through your Alumni account.
How can I login to AtoZ?
Upon exiting, you should have received an email invitation. However, if that is lost, you can set up your AtoZ Alumni account by entering your old username or personal email on the login page.
Start Dates
I need to reschedule my start date appointment.
Your start date is your orientation date after you’ve already attended your new hire appointment.
In order to reschedule your start date appointment, please contact us.
In order to reschedule your start date appointment, please contact us.
I had a start date appointment in the past, but could not attend and need to reschedule.
Your start date is your orientation date after you’ve already attended your new hire appointment.
In order to reschedule your start date appointment, please contact us.
In order to reschedule your start date appointment, please contact us.
Job Types
What types of jobs do you offer?
Amazon provides a variety of hourly roles for people interested in full-time jobs, part-time jobs, seasonal jobs, and even jobs with flexible schedules. Learn more to find the right job for you:
Warehouse – https://amazon.com/warehousejobs
Shopper – https://amazon.com/shopperjobs
Driver – https://amazon.com/driverjobs
Amazon Air – https://amazon.com/airjobs
Customer Service – https://amazon.com/csjobs
Locker+ – https://www.amazondelivers.jobs/about/locker-plus-jobs
Warehouse – https://amazon.com/warehousejobs
Shopper – https://amazon.com/shopperjobs
Driver – https://amazon.com/driverjobs
Amazon Air – https://amazon.com/airjobs
Customer Service – https://amazon.com/csjobs
Locker+ – https://www.amazondelivers.jobs/about/locker-plus-jobs
Customer Service Jobs
Where are Work-From-Home Customer Service jobs?
Amazon has Work-From-Home Customer Service jobs. To apply, you must live in the same country listed in the job description. If you don't see any work-from-home jobs listed in your country, there are no current openings.
Learn more:
Learn more:
Where do I find details on Customer Service Roles?
Visit this link to find out about the specific benefits, hiring process, and other details you may want to know.
Pay Rate and Benefits
What is the pay rate at Amazon?
$15 an hour is the Amazon minimum wage—although you can make more based on your location and the shift you choose.
Does Amazon offer benefits for hourly workers?
Amazon’s benefits can vary by location, the number of regularly scheduled hours you work, length of employment, and job status such as part-time, seasonal, or temporary employment.
Learn more about benefits at Amazon.
Learn more about benefits at Amazon.
When is pay day?
All hourly associates are paid on a weekly (every Friday) basis with 52 pay periods in each year.
Accommodations
Do you hire people with disabilities?
Amazon has always been, and always will be, committed to diversity and inclusion. We seek people from all backgrounds to join our teams.
Learn more about People with Disabilities hiring at Amazon.
Learn more about People with Disabilities hiring at Amazon.
General Questions
Who can I contact if I don't see my question?
If you have a question not listed here, including questions about hiring events, your job offer, or new hire paperwork, you can find answers or speak to a candidate support representative at https://hiring.amazon.com/contact-us
How do I opt-out of receiving SMS?
To opt out, you can change your contact preferences on the "Edit Profile" or "My Personal Information" section on the job portal.
What information do I need to provide if I was referred by someone?
You will be asked to provide the name and the Amazon login of the person who referred you. If you do not have the Amazon login, the person who referred you should be able to provide it to you.
I was referred by someone. Where do I enter the referral while completing the application?
You will be prompted to enter referral information after selecting the time slot for your New Hire Appointment after completing the application.
Ready to get started?
Sign up for job alerts.
Text NEWJOB to 31432*
*By participating, you agree to the terms and privacy policy at sms-terms.com/amazon for recurring autodialed marketing messages from Amazon, to the phone number you provide. No consent required to buy. Message and data rates may apply.
Text "STOP" to opt-out.

Amazon is committed to a diverse and inclusive workplace. Amazon is an equal opportunity employer and does not discriminate on the basis of race, national origin, gender, gender identity, sexual orientation, disability, age, or other legally protected status.
© 1996-2024, Amazon.com, Inc. or its affiliates